Pretty ominous headline1:
Fasting Until Noon Triggers Increased Postprandial Hyperglycemia and Impaired Insulin Response After Lunch and Dinner in Individuals With Type 2 Diabetes: A Randomized Clinical Trial
I am not a research scientist but respectfully disagree with the message this American Diabetes Association headline sends.
From the article:
CONCLUSIONS Skipping breakfast increases PPHG after lunch and dinner in association with lower iGLP-1 and impaired insulin response. This study shows a long-term influence of breakfast on glucose regulation that persists throughout the day. Breakfast consumption could be a successful strategy for reduction of PPHG in type 2 diabetes.
The ADA is consistent in their desire to have people eat from dawn to dusk, this headline is just another advocacy piece in the same vein. The study is set up to measure the values of two DIABETIC groups, those who eat three meals (YesB) and those who skip breakfast (NoB) so eat just two meals. Let’s unpack their key takeaways.

PPHG is postprandial hyperglycemia, so they show a little higher glucose after the two meals in the NoB group, about 9% in AUC. A little more glucose around, but an important point to emphasize here is these are diabetics, and they are given meals that are over 50% carbs. It is amazing we have to continue to explore studies where we are measuring how bad responses might be to meals of bad macronutrient compositions.
Impaired Insulin Response
Wording matters.
impaired | imˈperd |
adjective
1 weakened or damaged
Is having less insulin IN DIABETICS bad (or weak or damaged). I think not.
In diabetes, high blood sugar is just part of the issue. A critical amount of the downstream consequences diabetics face is having high levels of insulin resultant from the body’s efforts to get all the glucose out of the bloodstream and the cells listening less and less, a condition called insulin resistance, which the ADA has a little info out there on2:

They point out correctly, that insulin resistance causes problems. To reverse, they say to eat less calories, but according to the article not too few (like 0 for breakfast)?
So, if insulin resistance is bad, improving insulin sensitivity, or to use the language of the headline reducing its response, would be good right?
The graphs above, the one with B, clearly shows they saw less insulin in the no breakfast group in total throughout the day; 30% less by AUC (area under the curve). Isn’t that a good thing? I have written a touch on insulin where it is problematic for Alzheimer’s and is a key signaling hormone for the growth pathway mTOR (which is implicated in cancer). To me, skipping breakfast is a clear victory in the study by reducing insulin.
Intermittent fasting (IF) or Time Restricted Eating (TRE) where the strategy is shrinking the eating hours boasts many benefits. One of them is reducing insulin resistance, as the ADA study shows despite its scary headline.
This study3 demonstrated recently in the TRE method where dinner is skipped vs breakfast (my assessment is the results would be the same or very similar if breakfast was skipped as long as there were at least 3 hours fasting before bed included in the design), but the benefits are pronounced.
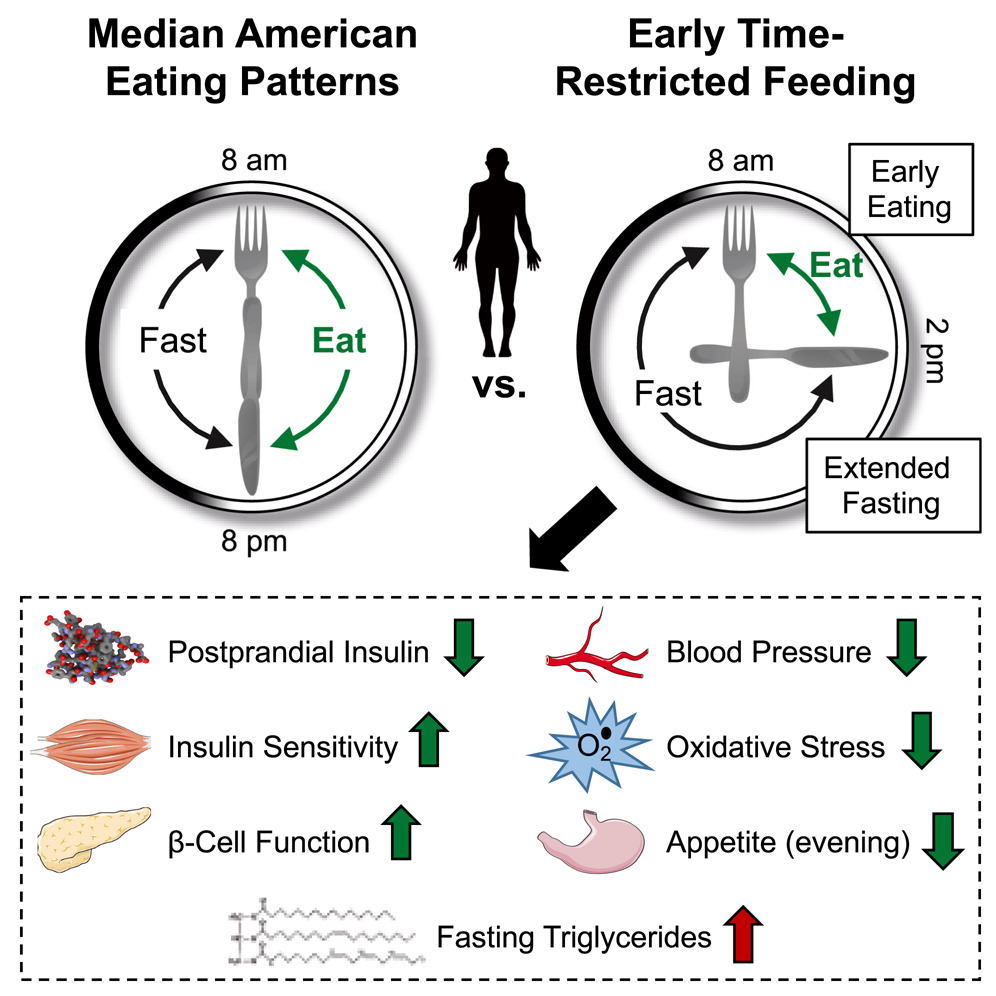
Early Time-Restricted Feeding Improves Insulin Sensitivity, Blood Pressure, and Oxidative Stress Even without Weight Loss in Men with Prediabetes
Increased Fat in the blood
Moreover, the higher plasma glucagon levels are associated with increased triglyceride breakdown in adipose tissue leading to a further increase in plasma FFA levels, aggravating the higher glycemic response described above.
As the original ADA article, and the image above show, there is an increase in Free Fatty Acids (FFA) in the blood. It is construed as a negative, but let’s look at that a little closer; “breakdown in adipose tissue”. Fancy terminology for fat burning!
As predicted, if we have breaks in eating there is less insulin. When there is less insulin, the fat cells aren’t told to store fat. This means it can be used as fuel, a good thing. Fat cells are very much binary in how they operate on store/accumulate vs burn/reduce spectrum. The master controller of which state they are in is insulin. Reducing insulin is a good thing and a key to improving the health of diabetics.
Why the tone from the headline?
When I first saw that article in my feed, I did a double take. The headline was exactly the opposite of the information I had seen and experienced myself. I then saw the ADA involvement and took it with a grain of salt (which is also a good thing despite what the American Heart Association will tell you!). The ADA is funded primarily by those who benefit from the condition itself. Further, I’m sure one of its $100k level companies, Dannon Light & Fit, appreciates the message of don’t skip your breakfast.


Leave a Reply